The role of explicit bias in working with depressed cardiac patients
Living with a heart disease can be stressful. After all, a well-functioning heart is vital, and it can be tough to realize that your heart is failing. Coronary artery diseases (CAD) can often lead to experiences of psychological problems, such as becoming anxious and feeling tired or lifeless, with the possibility that depression can occur or get worse.
In addition, depression can lead to a greater chance of developing a CAD as well. As there is a strong link between our physical health and our mental health, it should not come as a surprise that depression is an independent risk factor for CAD and its complications, and CAD in turn can be a cause of depression.
Physicians’ attitudes towards depressed patients
Unfortunately, evidence suggests a lack of awareness of such links between mental and physical conditions among physicians, especially in cases where the mental illness is complex and accompanied by communication or behavioral challenges that interfere with the clinical presentation.
However, once physicians become aware of their attitude towards such patients, it is possible to modify their behavior with education, motivation, skill, and cognitive resources.
In order to explore this topic further, Dr. Kathleen Crapanzano and her team conducted a study to explore the role of explicit bias in medical students’ diagnoses and treatment plans for a standardized patient (SP) presenting as mildly depressed. They then compared these students’ performance with medical students encountering an SP without depression.
Simulating medical encounters to measure the influence of bias
Crapanzano and her team intended to answer three questions in this study:
- What is the incidence and degree of internal medicine students’ extrinsic bias toward patients with depression as measured by the Medical Condition Regard Scale (MCRS)?
- What relationships, if any, exist between medical students’ MCRS scores and objective structured clinical exam (OSCE) evaluation scores?
- What differences in OSCE performance and facial expressions are observed in medical students who encounter a depressed SP compared to medical students who encounter a non-depressed SP?
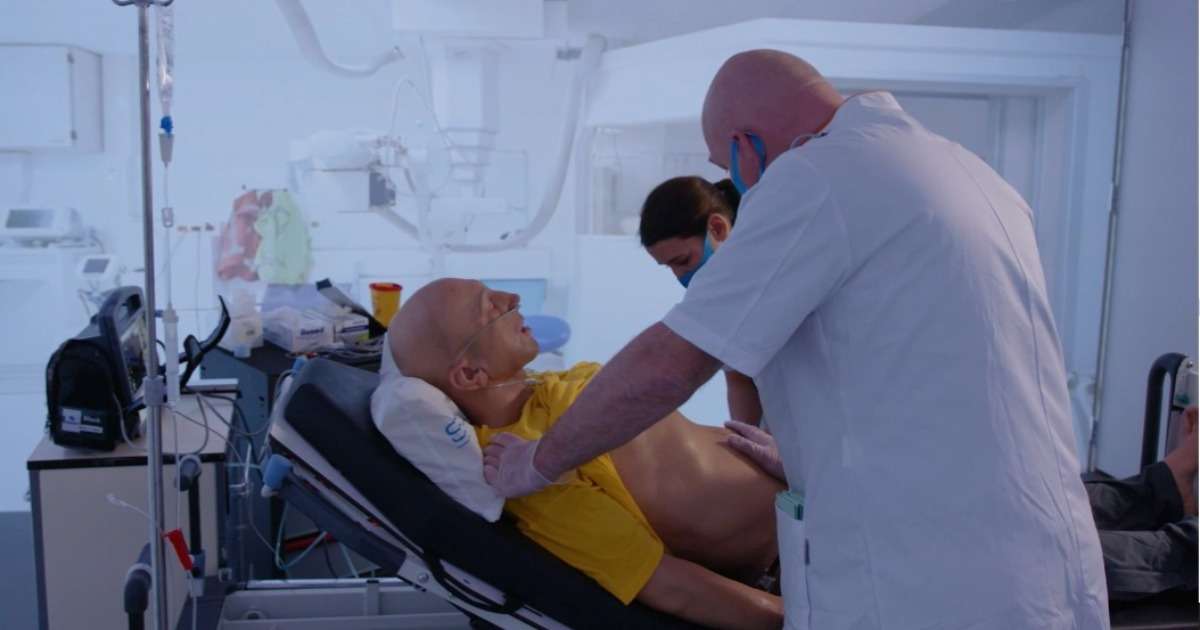
The randomized controlled trial included 185 internal medicine students (97 of these students were placed with the depressed SP-group). All SPs were actors who portrayed a patient with acute chest pain. Half of the SPs were also trained on symptoms of depression. However, they were instructed not to mention their depression unless specifically asked about it by the students.
Measuring students’ facial expressions when meeting with depressed patients
Within 15 minutes, the medical students were instructed to obtain a history, perform a physical examination, and inform the SP about their diagnostic impression and treatment plan. Afterwards, the SPs completed the OSCE checklist in order to assess the students.
All clinical exams were videotaped and analyzed using FaceReader to measure the facial expressions of the students.
The medical students completed a structured post-encounter note (PEN) that described their primary diagnoses and workup plan, and a questionnaire (MCRS) to measure their self-reported extrinsic bias toward depressed patients.
Working with depressed patients releases feelings of disgust
The researchers found an overall low regard towards patients with depression in both groups of students. However, the results of the study did not support the hypothesis that this low regard was related to the students’ performance during the simulated clinical exam. The students may have been aware of their biases while examining and treating the patients during the simulated encounter, and could have suppressed these feelings.
The students who worked with the depressed patients showed more occurrences of the disgust affect while students who worked with non-depressed patients showed more occurrences of a neutral affect. Crapanzano and her team also found differences within gender groups. Male students were more likely to demonstrate an angry affect, while female students were more likely to show a sad or scared affect and express feelings of empathy.
In conclusion, the researchers recommend conducting further research to examine the effects of patient mental health conditions on physician examination procedures, diagnostic behaviors, and patient outcomes.

Interested in human behavior research? Read more on 'How to study human behavior'!
References
- Crapanzano, K.; Fisher, D.; Hammarlund, R.; Hsieh, E.P. & May, W. (2018). Internal Medicine Residents’ Attitudes Toward Simulated Depressed Cardiac Patients During an Objective Structured Clinical Examination: A Randomized Study. Journal of General Internal Medicine, 33 (6), 886-891. DOI: 10.1007/s11606-017-4276-7
- Jones, S.; Howard, L.; Thornicroft, G. (2008). Diagnostic overshadowing: worse physical health care for people with mental illness. Acta Psychiatrica scandinavica, 118 (3), 169–71.
- Merrick, J.; Merrick, E. (2007). Equal Treatment: Closing the Gap. A Formal Investigation into Physical Health Inequalities Experienced by People with Learning Disabilities and/or Mental Health Problems. J Policy Pract Intellect Disabil, 4(1), 73.
Get the latest blog posts delivered to your inbox - every 15th of the month
more
What is simulation-based training?
Simulation-based training provides learners with an opportunity to test out different scenarios to see what works and to understand how they arrived at the right and wrong answers.
Implementing Tailored Activity Programs
Tailored Activity Programs (TAP) have been shown to have significantly reduce behavioral occurrences in dementia patients and improve engagement and positive behaviors.