How to assess medical team effectiveness
Healthcare professionals working in an operating or emergency room, frequently deal with unpredictable situations in which they need to stay focused and think clearly. How do they manage that?
Posted by
Published on
Thu 20 Jun. 2019
Topics
| Healthcare | Medical Encounter | Medical Simulation | Teamwork | The Observer XT |
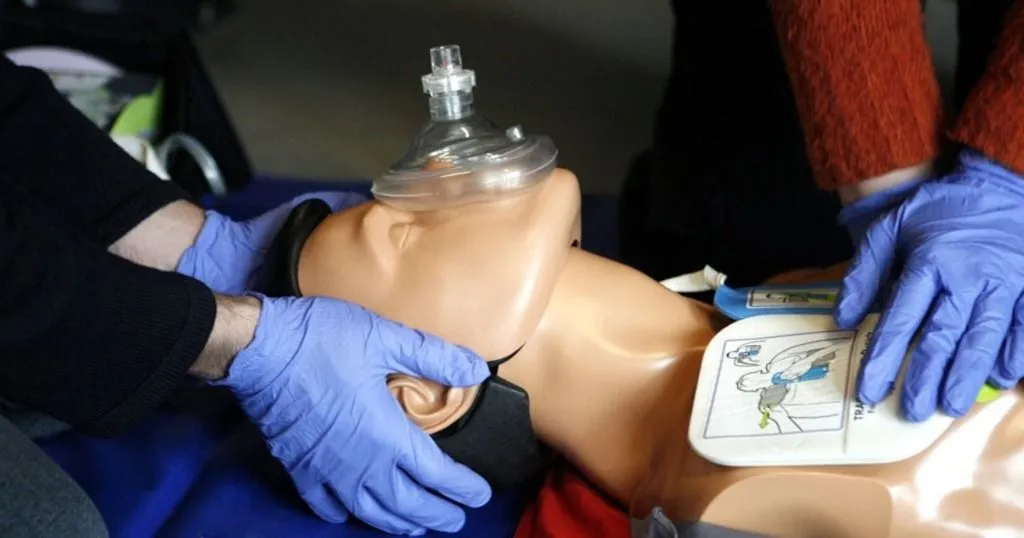
Everyone knows that it is hard to stay focused and think clearly when you are in a very stressful situation. However, when that situation is all about saving someone’s life, that is exactly what you need to do: stay focused and think clearly.
Healthcare professionals, particularly in the operating or emergency room, deal with this all the time. In unpredictable situations, they need to carry out complex medical procedures. Then, effective teamwork is of the utmost importance.
This means there must be effective communication, coordination of activities, clarity on decision making, and managing of errors. These aspects will all influence the outcome of the crisis.
Multiple data streams can be used to measure team effectiveness
The performance and effectiveness of teams has been the focus of many researchers. On our Behavioral Research Blog, we already mentioned a few studies. In this blog post, the spotlight is on the study of Hoogeboom and colleagues from the University of Twente, The Netherlands, which was performed in a medical simulation room for advanced life support (ALS) training.
ALS is a complex emergency situation following the cardiac arrest of a patient, and is characterized by “extreme time pressures, diagnostic uncertainty, and rapidly evolving situations.” [1]
In their study, the researchers combined different research methods:
- Video observation: to systematically analyze the content of team interaction behaviors
- Innovative sensor technologies: to explore the structure of team interaction processes in more detail and identify moments of high arousal
- Surveys: to assess team effectiveness
The study sets out to uncover what the added value, pitfalls, and hurdles are when using and combining different sensor technologies with additional measures in order to better understand team interactions. They claim that outcomes of their research will help optimize simulation-based team trainings, and thus improve the medical and interactions skills of healthcare professionals.
What’s the big picture?
Twenty-one teams, consisting of four first-year master’s students, participated. During the ALS course, students learned to diagnose and manage a patient with cardiac arrest and perform cardiopulmonary resuscitation (CPR) on an advanced human-patient simulator [2].
All four students of each team were randomly assigned to these fixed team roles:
- Team leader - responsible for task distribution, monitoring team performance, creating an overview of the situation, and patient handover at the end of the scenario
- Medication nurse - responsible for drug administrations and connecting devices to the patient
- Two CPR administrators - responsible for chest compressions and airway management
They all wore a sociometric badge, which is a wearable device that measures proximity, body movement and speech features.
In addition, a wristband was placed on the wrist of the team leader’s non-dominant hand to help record skin conductance responses and consequently detect the moments of high arousal. In the context of medical simulations, higher levels of arousal may arise when time pressure forces an ALS team member to act quickly.
The content of the team interactions was coded with The Observer XT. Behaviors such as giving a command, summarizing, confirming, and asking questions were collected by the team leader. The remaining three team members were only coded on checking back with the team leader.
FREE TRIAL: Try The Observer XT yourself!
Request a free trial and see for yourself how easy behavioral research can be!
- Work faster
- Reduce costs
- Get better data
Finally, to assess team effectiveness, two teachers scored on four effectiveness items directly after the simulation was finished: “This team is a consistently well performing team,” “This team is effective,” “This team makes few mistakes,” and “This team delivers high quality work.” As a result, the teams were categorized as ‘more’ or ‘less’ effective.
Team interaction during stressful moments
Regarding the content of the team interaction, the results showed that in the beginning of the scenario, the team leader expressed many commands. However, at the end of the scenario, when teams had to reach a diagnosis and handover the patient, there was more communication back and forth.
Moreover, in the more effective teams, one person was more dominant in terms of speaking time, while in less effective teams the team members contributed more equally. On average, more effective teams were less imbalanced during moments of high arousal. During those moments of high arousal, team leaders mostly gave commands and asked less often for confirmation or opinions. They also made fewer suggestions.
Stay focused and think clearly
It is crucial for an ALS team to be well organized so that individual skills can be deployed efficiently and effectively. Therefore, understanding team interactions is key. The authors conclude in their article:
“This and future studies might enable future medical professionals to better understand what is required at stressful moments. Using these results in training and during debriefing sessions can potentially optimize team interactions of future medical professionals and enhance the quality of medical care.”
References
- Doumouras, A. G., Keshet, I., Nathens, A. B., Ahmed, N., & Hicks, C. M. (2012). A crisis of faith? A review of simulation in teaching team-based, crisis management skills to surgical trainees. Journal of Surgical Education, 69 (3), 274-281. https://doi.org/10.1016/j.jsurg.2011.11.004
- Endedijk, M.; Hoogeboom, M.; Groenier, M.; Laat, S. de & Sas, J. van (2018). Using sensor technology to capture the structure and content of team interactions in medical emergency teams during stressful moments. Frontline Learning Research, 6 (3), 123-147. https://doi.org/10.14786/flr.v6i3.353
Related Posts

Mealtime challenges in dementia: insight in difficulties

The role of emotional expressions after face transplant
