Does the sex of a simulated patient affect CPR?
When faced with either a male or female patient simulator, both men and women rescuers appeared reluctant to remove a female patient simulator’s clothing.
Posted by
Published on
Mon 20 Apr. 2015
Topics
| Doctor-patient Interaction | Education | MediaRecorder | Medical Encounter | Simulation | The Observer XT |
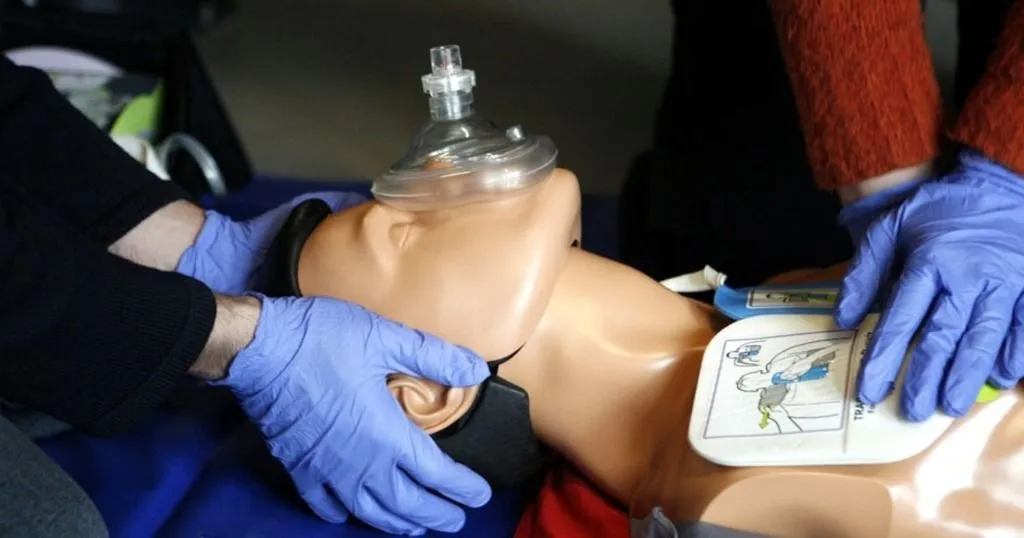
It shouldn’t, but it does.
Although men and women are equally at risk for sudden cardiac arrest, studies have found that women are less likely to be resuscitated – by both bystanders and medically-trained personnel.
Chelsea Kramer and her colleagues discovered that in the experiment they set up, when faced with either a male or female patient simulator, both men and women rescuers appeared reluctant to remove a female patient simulator’s clothing, with men being significantly more hesitant to do so. However, the hand placement for CPR on the female was more ideal compared to on the male simulated patient.
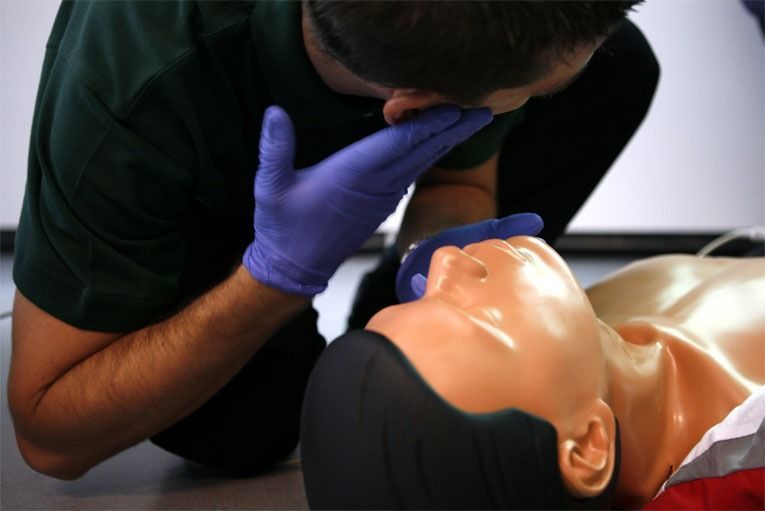
Out-of-hospital cardiac arrest
Kramer and colleagues conducted their study in the Healthcare Human Factors and Simulation Laboratory (HHFSL) at the University of Calgary’s W21C Research and Innovation Centre. They invited 69 participant to the lab and set up two scenarios: an out-of-hospital cardiac arrest (OHCA) with a male simulated patient and an OHCA with a female simulated patient.
Reviving a cardiac arrest patient
The patient simulator, “iStan,” was used in the control condition. The same simulator was transformed from the male iStan into the female patient “iSam” with the addition of a wig, make-up, silicone breasts, a front opening brassiere, and color-coordinated women’s clothing; for this experiment, test participants were randomly assigned to either the male or female simulator.
Upon arrival to the test site, each participant was introduced to the patient simulator and told that he/she would be rescuing an unconscious patient. Then, the OHCA scenario began when the participant found either iStan or iSam in an apparent state of shock; the participant was given an AED and barrier mask and tasked with the resuscitation of the patient. Once activated, the AED instructed the participant in performing CPR on the patient by providing chest compressions and rescue breaths, resulting in an eventual recovery of the simulated patient.
Following the OHCA scenario, participants were interviewed about their experience, including how they felt about removing the patient’s clothing and their discomfort and reservations, if any, in doing so.
Removing clothing and planting down hands
Participants were observed live through a one-way mirror at the same time that video/audio recordings were being made for detailed analysis afterwards. The recordings were triggered via the Noldus MediaRecorder software, coded in The Observer XT, and analyzed with IBM SPSS. The researchers primarily focused on the percentage of rescuers who completely removed clothing from the simulated female patient’s chest compared to the male’s, and the placement of rescuers’ hands when CPR was initiated.
Hand placement
So what is considered good hand placement?
Kramer and colleagues explain that initial hand placement in CPR is important and should be centered on the chest, as compressions outside of the “red zone” can result in harm.
On iStan, hand placement of both male and female rescuers was scattered across the chest. In contrast, on iSam, the rescuers’ hands tended to be centralized between the breasts. They either chose to avoid touching the breasts or used the breasts as ‘landmarks’ to aid in placing the hands in the correct position.
Disrobing the patient
After the experiment, the participant video data was analyzed to find the relationship between patient sex and rescuer sex. While the researchers found no difference between the men and women rescuers in baring iStan’s chest, men were significantly less likely to remove iSam’s clothing than were women; only a couple of men removed her brassiere, and only 14 out of all the rescuers removed both the blouse and the brassiere.
Interviews with the rescuers revealed that, despite clear AED instructions for complete clothing removal for proper CPR, most participants thought they only needed to remove enough clothing to place the defibrillator pads. The reluctance to reveal iSam’s chest was most commonly pointed towards social norms and a concern for patient modesty.
How can we improve patient care?
Reasons for why female OHCA patients are less likely to be resuscitated than men have thus far only been suggested, not supported by data. In comparing the iStan and iSam results, Kramer et al. emphasize the importance of using realistic female patient simulators in CPR training: Up to this point, CPR training and research typically tend to use a single type of mannequin, which is described as having “perceived low levels of realism.”
Kramer’s study suggests that unrealistic simulator models are insufficient for training medical professionals – much the general public – to deal with complex social norms and adequately tend to patients in case of emergencies.
Further research is suggested to find effective ways to overcome societal and cultural inhibitions, and provide better care for female patients.
Reference
Kramer, C.E.; Wilkins, M.S.; Davies, J.M.; Caird, J.K.; Hallihan, G.M. (2015). Does the sex of a simulated patient affect CPR?Resuscitation, 86, 82-87.
Image by Rama (Own work) [CeCILL (http://www.cecill.info/licences/Licence_CeCILL_V2-en.html) or CC BY-SA 2.0 fr (http://creativecommons.org/licenses/by-sa/2.0/fr/deed.en)], via Wikimedia Commons
Related Posts
Improving patient safety
Evaluating the effectiveness of simulation in healthcare

