Gait recovery and other effects: treatment of cervical myelopathy
At the Dr. Michael Fehlings' lab, they are on a quest to find out what exactly causes the lower success rate of delayed surgery in cervical myelopathy.
Posted by
Published on
Thu 22 Jun. 2017
Topics
| CatWalk XT | Gait | Gait Analysis |

Degenerative cervical myelopathy (DCM); a mouthful to describe what happens when the spinal cord and blood vessel become compressed and causes all kinds of neurological symptoms such as clumsy hands, unstable gait, and sensory changes in arms.
Degenerative cervical myelopathy
DCM encompasses a spectrum of arthritic and ligamentous conditions of the cervical spine, such as Cervical spondylotic myelopathy (a neck condition). It is the most common cause of non-traumatic spinal cord injury, is often age-related, and happens mostly to older patients. Clinical signs vary, and can include loss of manual dexterity, pain and impaired gait.
Decompression
The good news is that the standard treatment, surgical decompression, can halt the progression of the disease and improve neurological and functional status dramatically. The bad news is that symptoms are not always recognized quickly, and the success of the surgery seems to largely depend on how soon it takes place after symptoms started, how young the patient is, and the comorbidities patients present before surgery.
Success rate of surgery
Pia Vidal and her colleagues from Dr. Michael Fehlings' lab, are on a quest to find out what exactly causes the lower success rate of delayed surgery. In previous work (Karadimas et al., 2015), her colleagues found ischemia-reperfusion injury (IRI) to be a key factor in the neurological decline in rat models after decompression surgery. However, the role of inflammation in this process was unclear.
Mouse model
Vidal’s recent paper in JCI Insight describes the study of a mice model with C5-C6 compression (the most common site for DCM in the spinal segment in patients), comparing the results of early versus late decompression. They show that the restoration of the spinal cord blood flow after surgery runs in parallel with an acute activation of an immune response, however, the duration of response does differ between the early and late decompressed subjects.
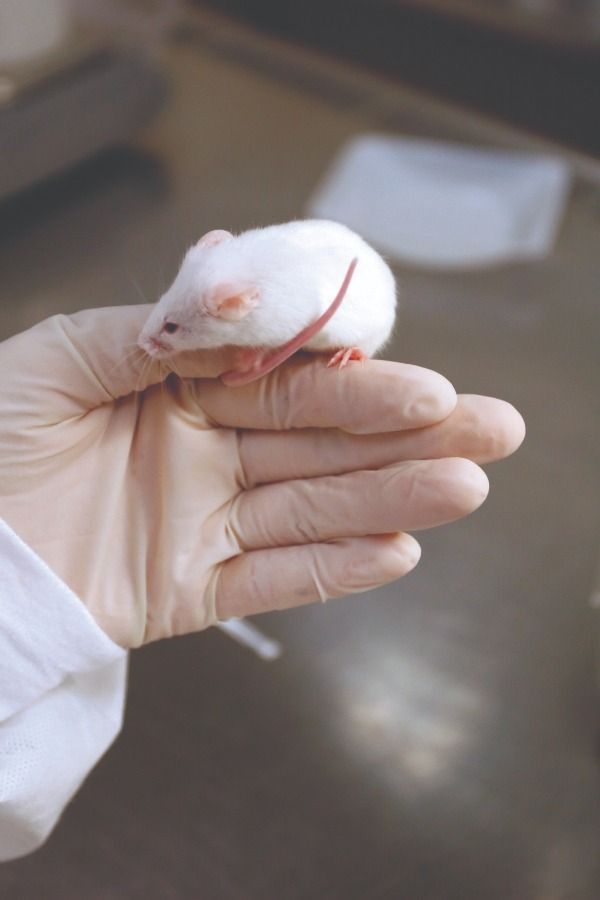
Prolonged immune response
When surgery is performed early the acute activation of the immune system is resolved within the first weeks, whereas after delayed surgery there is a prolonged response. This response is characterized by increase cell signaling (more cytokines in the spinal cord), in the number of astrocytes (a cell type that supports and protects neurons), and in the number of peripheral monocytes (white blood cells).
As expected, mice that received late decompression showed more complications and less recovery after surgery, potentially due to this ongoing unresolved activation of the immune response associated with a longer duration of symptoms. Early decompression resulted in neurological improvement in upper and lower limbs.
Functional recovery of gait
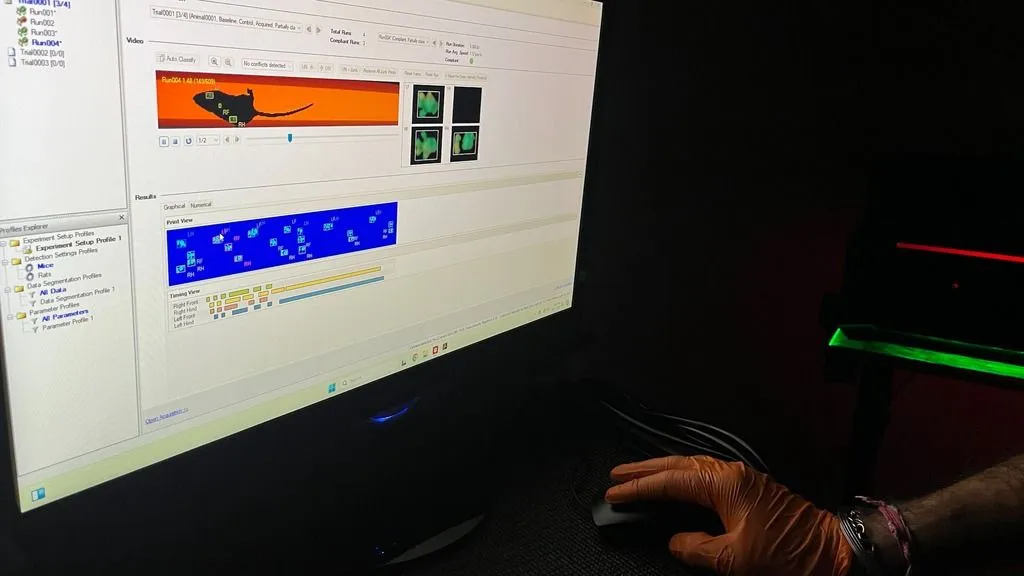
Gait impairment in one of the first symptoms in patients with DCM, so for this study, the assessment of gait was important to measure functional outcomes. Using the CatWalk XT method, swing speed and stride length, similar to what is affected in patients, were measured in all mice.
In the first two weeks after surgery, this revealed no differences between the mice. At five weeks after surgical decompression, mice that received early decompression showed significant improvement, while the other did not benefit that much from the surgery.
Vidal also investigated interlimb coordination and found pattern and speed to be visibly affected in all mice. After surgery, the early decompression cohort showed much more improvement in step patterns than the others.
Novel therapeutic target
This study underlines the importance of early diagnoses of DCM. The IRI and inflammation mechanism plays an important role in the poor functional outcomes of delayed surgery, and thus presents a novel therapeutic target to improve this.
References
- Fehlings, M.G.; Wilson, J.R.; Kopjar, B.; Yoon, S.T.; Arnold, P.M.; Massicotte, E.M.; Vaccaro, A.R.; Brodke, D.S.; Shaffrey, C.I.; Smith, J.S.; Woodard, E.J.; Banco, R.J.; Chapman, J.R.; Janssen, M.E.; Bono, C.M.; Sasso, R.C.; Dekutoski, M.B.; Gokaslan, Z.L. (2013). Efficacy and safety of surgical decompression in patients with cervical spondylotic myelopathy: results of the AOSpine North America prospective multi-center study. The Journal of Bone and Joint Surgery.95(18), 1651-1658.
- Nouri, A.; Tetreault, L.; Singh, A.; Karadimas, S.K.; Fehlings, M.G. (2015). Degenerative Cervical Myelopathy: Epidemiology, Genetics, and Pathogenesis. Spine (Phila Pa 1976), 40(12), e675-693.
- Karadimas, S.K.; Laliberte, A.M.; Tetreault, L.; Chung, Y.S.; Arnold, P.; Foltz, W.D.; Fehlings, M.G. (2015). Riluzole blocks perioperative ischemia-reperfusion injury and enhances postdecompression outcomes in cervical spondylotic myelopathy. Science Translational Medicine, 7(316), 316a194.
- Vidal, P.M.; Karadimas, S.K.; Ulndreaj, A.; Laliberte, A.M.; Tetreault, L.; Forner, S.; Wang, J.; Foltz, W.D.; Fehlings, M.G. (2017). Delayed decompression exacerbates ischemia-reperfusion injury in cervical compressive myelopathy. JCI Insights, 2(11), e92512.
Acknowledgements
A big thanks to Pia Vidal for providing information about her research. Go check out Dr. Michael Fehlings' lab at http://www.drfehlings.ca and follow Dr. Fehlings on Twitter @DrFehlings
Other research with CatWalk XT:
Related Posts

Rat strain and sex matter in spinal cord injury research: insights from CatWalk XT
FAQ: tips and tricks for CatWalk XT

